-
-
Featured Care Areas


Source: Shutterstock
Slipped Discs: Causes, Symptoms & Treatments
Last updated: Monday, January 24, 2022 | 5 min reading time
Having constant back pain that worsens with certain movements? There's a chance it may be a slipped disc. Dr Mashfiqul Siddiqui, orthopaedic surgeon at Parkway East Hospital, shares on causes, symptoms, and treatments available.
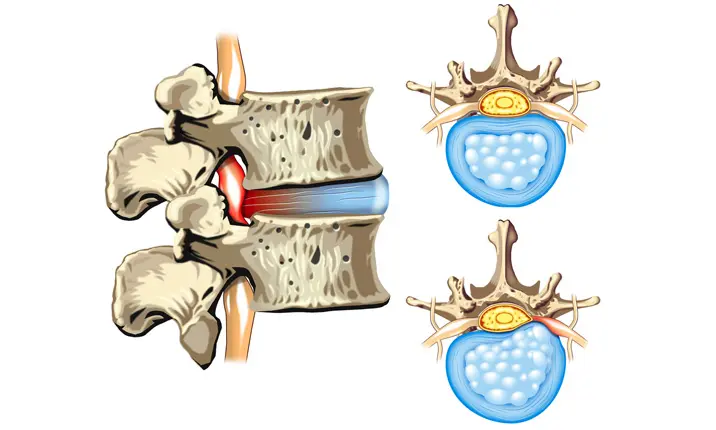
The spine is composed of multiple bones, known as vertebrae, and soft, jelly-like cushions, known as intervertebral discs. As the bones move along the facet joints, located at the back of the vertebrae, the discs help to distribute the load, acting as shock absorbers. In a normal spine, the discs should remain within a confined space between the bones, held in place by fibrous tissues that keep the gel contained. There are also nerves that lie behind the vertebrae and the discs, controlling your arms, legs and bladder function.
What is a slipped disc?
A slipped disc, also known as a herniated nucleus pulposus, occurs when the disc material moves (or slips) out of its normally defined space, irritating the surrounding nerves and causing a host of painful symptoms. This tearing of the tissues around the disc can happen when your back is under extra strain, such as when you are carrying a heavy load, or making a sudden movement.
Slipped disc symptoms
If you're experiencing the following, it could be a slipped disc:
- Pain at the site of the slipped disc, eg. neck pain if the disc is in the neck, or lower back pain if the disc is in your lumbar spine
- Tingling or numbness, which occurs if the disc is touching your nerves
- Shooting pains in your arms or legs
- Weakness in your limbs or hands
- Loss of balance or coordination
- Issues with your fine motor skills
- Difficulty passing urine, known as urinary retention
The severity of your symptoms depends on where the slipped disc is protruding from and whether it is touching your nerves or pressing on your spinal cord.
Diagnosing a slipped disc
If you have any of the symptoms of a slipped disc, it's important to visit an orthopaedic specialist, particularly if you are suffering from nerve dysfunction (tingling, numbness, sciatica or urinary retention). Your doctor will provide you with a full examination, and any scans or tests required to determine a diagnosis.
The best form of imaging to diagnose a slipped disc is usually an MRI, also known as magnetic resonance imaging, which can create detailed 3D images of the spine. An x-ray might be used to rule out other causes of the pain, such as a fracture, but will not be able to show if you have a herniated disc. If your doctor doesn't perform an MRI, there are other tests you might undergo, such as a CT scan, or a myelogram, which is a test using dye injected around your spinal cord and imaging to locate pressure on your spine.
If your doctor thinks your nerves are damaged, they might also order further tests, such as an electromyogram or nerve conduction studies, to check the activity of your nerves.
Treating a slipped disc
Fortunately, slipped discs can often be treated with medication, physiotherapy and activity modification. Some of the most common treatment options are:
Rest
Getting plenty of rest can help reduce swelling, allowing your spine time to heal itself. You do need to keep moving to some degree to prevent stiffness, but reduced activity with no heavy lifting is a good way to improve symptoms of your slipped disc.
Physical therapy
Physiotherapists can work with you to create a programme that helps with your recovery and keeps you mobile. This might include stretching, gentle aerobic exercise, ultrasound, massage, or heat and cold therapy.
Medication
Over-the-counter anti-inflammatories and painkillers can help. However, you should consult your doctor before you take anything, especially if it's for more than 1 – 2 days. In more severe cases, your doctor might prescribe stronger painkillers, muscle relaxants or nerve pain medication, if required.
Injections
Steroid injections are sometimes used at the site of the pain to ease swelling and reduce pain.
Slipped disc surgery
Most patients with a slipped disc will heal within a few weeks, using one or a combination of the above treatment options to aid their recovery. However, surgical treatment may sometimes be needed to prevent further nerve damage.
Dr Mashfiqul explains: "Modern surgical treatment of the slipped disc in the lower back has an excellent outcome. Decompression of the nerve through surgery and removing the fragment responsible for the problem can be done through minimally invasive techniques or keyhole surgery."
This approach involves making a small cut in the patient's back and using a microscope to remove the loose piece of the disc and free the nerve. This process is safer than more invasive techniques, with rapid recovery time and very little pain. For slipped discs in the neck, the fragment can be removed from the front of the neck through a skin crease incision, once again using a microscope for better visualisation.
"After removal of the offending disc, an artificial disc replacement or a fusion of the segment can be done," says Dr Mashfiqul. "Like lower back surgery, modern spinal surgery of the neck is very safe, with rapid recovery from surgery and high patient satisfaction rates."
Preventing slipped discs
Whether you are prone to back pain or not, you should take steps to ensure you look after your spine. Doctors recommend the following to maintain a healthy spine:
Focus on your posture
Try to keep your back straight when sitting or standing.
Maintain a healthy weight
Being overweight can add unnecessary stress to your joints and can increase pressure on your back.
Exercise regularly and stay mobile
Exercising your core muscles – those located in your lower back and abdomen – will give more support to your spine.
Quit smoking
Smoking can affect the blood supply to the disc and damage it.
Practise safe lifting techniques
Lifting heavy objects can potentially hurt your back if done the wrong way. It is therefore important to ensure that you are doing the lifting the right way. When picking something up, bend your knees. Then, keep your back straight when lifting. Ask for assistance if the load is too much for one person to lift.
Ensure proper support when sleeping
Having a good mattress is important. Use a firm or medium-firm mattress to support the spine rather than one that is too soft and allows the spine to sag.
And remember, if you are suffering from severe back pain, it's important to see an orthopaedic specialist to determine the cause.
Felson, S. (2016, December 17) What is a Herniated Cervical Disk? Retrieved October 30 2018 from https://www.webmd.com/pain-management/what-is-a-herniated-cervical-disk#2
Martin, L.J. (2016, October 9) Do I have a Herniated Disk? Retrieved October 30 2018 from https://www.webmd.com/pain-management/do-i-have-a-herniated-disk#2
Martin, L.J. (2016, October 9) What are the Treatments for a Herniated Disk? Retrieved October 30 2018 from https://www.webmd.com/pain-management/treatments-for-herniated-disk#3
Martin, L.J. (2016, October 9) Do I have a Herniated Disk? Retrieved October 30 2018 from https://www.webmd.com/pain-management/do-i-have-a-herniated-disk#2
Martin, L.J. (2016, October 9) What are the Treatments for a Herniated Disk? Retrieved October 30 2018 from https://www.webmd.com/pain-management/treatments-for-herniated-disk#3