Dr Shim Hang Hock
Gastroenterologist


Source: Shutterstock
Gastroenterologist
Gastroesophageal reflux disease (GERD) – more commonly known as acid reflux – is a condition where the contents in your stomach backflows up into your oesophagus regularly, causing bothersome symptoms, and can even damage the oesophagus.
When we swallow, food travels down the oesophagus to the stomach through a rhythmic wave of contraction, also known as peristalsis. The lower oesophagus sphincter, a muscular ring which sits at the bottom end of the oesophagus subsequently relaxes, allowing food to pass through. Once the food enters the stomach, the muscle contracts to prevent food and stomach acid from going back up the oesophagus.
However, these sphincter muscles may sometime weaken and allow stomach acid to backflow regularly, irritating your oesophagus lining.
The common symptoms of GERD are:
In some patients, they may have atypical symptoms as a result from GERD, such as:
Long term acid reflux may result in injury to the oesophagus, also known as oesophagitis. If severe, stricture or narrowing of the oesophagus may occur, which results in difficulty for food to travel down the oesophagus.
In rare instances, patients may even develop a precancerous condition known as Barrett’s oesophagus, which carry a very low risk of progression to oesophageal cancer.

Certain conditions increase the risk of GERD. They include:
There is an increased prevalence of GERD among individuals who are overweight or obese. The reason for this is not completely understood but experts think that excess belly fat may be adding pressure to the abdomen, causing fluid to backflow into the oesophagus. Being overweight can also impair your stomach’s ability to empty properly.
A significant number of pregnant women report having serious heartburn, especially during their second and third trimesters. This may be due to hormonal changes and the growing baby pressing against your stomach.
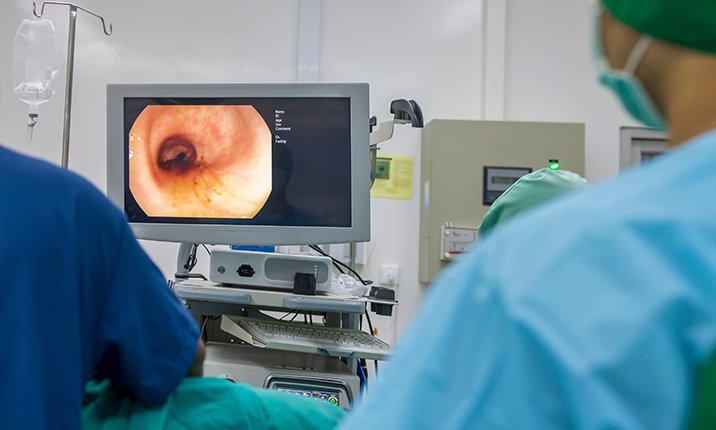
Diagnosis of GERD is usually made based on typical symptoms. Your doctor may recommend further tests such as:
Gastroscopy is a flexible endoscope which allows your doctor to examine the internal lining of your oesophagus and stomach. This may be necessary to assess the damage caused by acid reflux and to look for any complications such as ulcer, narrowing, or cancerous growth.
A long, thin, flexible tube fitted with sensors will be inserted through the nose into the oesophagus. Over the course of 24 hours, it will measure any acid reflux event in the lower oesophagus. This allows your doctor to confirm the acid reflux and to correlate with your symptoms.
For more ways to diagnose GERD, visit this page.
Seek immediate medical attention if:
GERD can be managed successfully for majority of patients via a combination of lifestyle modification and over-the-counter medications. However, if your GERD symptoms don’t improve, your doctor might recommend prescription medications, or in some cases, surgery.
Over-the-counter medications, such as antacids, work by neutralising the gastric acid.
If your symptoms are persistent, your doctor may prescribe the following medications which work by reducing acid production:
These medications are generally safe, and your doctor will discuss with you in detail should your symptoms warrant the use of medication. Treatments are usually intended to control symptoms using as small a dose of medication as possible, and tailored according to the frequency and severity of symptoms.
Various endoscopic and surgical procedures have been invented to treat GERD via artificially increasing the lower oesophageal sphincter pressure. These generally have a limited role as a majority of patients with GERD can be treated effectively with lifestyle modifications and medications. Example of endoscopic therapies include:
In this procedure, a medical device is inserted through your mouth to create folds at the distal oesophagus. A barrier is thus created between the stomach and the oesophagus, preventing acid reflux.
This procedure uses radiofrequency energy which is delivered to the distal oesophagus. The thermal injury reduces tissue compliance and therefore achieves the target effect of reduced relaxation of the lower oesophageal sphincter.
Fundoplication is a surgical procedure where the upper part of stomach is wrapped and stitched together at the lower oesophagus. This strengthens and increases the pressure at the lower oesophagus sphincter, thereby reducing acid reflux.
Patients with an abnormal pH study and who do not respond to or are intolerant of medical treatment can consider this treatment option.
If you suspect that you may be suffering from GERD, consult a gastroenterologist for an evaluation.
From persistent heartburn to complex liver conditions, digestive issues can affect your comfort and confidence in daily life. At Gleneagles Hospital, our experienced team brings together advanced diagnostics and compassionate, coordinated care — all under one roof. Start your journey towards digestive well-being today.
Find a specialist